|
|
|
|
|
|
Provider Services 1-833-644-6001 |
|
|---|
|
|
2025 Provider Satisfaction Survey
Thank you for your continued partnership with AmeriHealth Caritas Ohio in the service of our members. We recognize how critical your role is in providing and coordinating care.
Please watch for our upcoming satisfaction survey mailed by our partners at Qualtrics. It will be mailed to randomly selected providers for anonymous feedback and should take no more than 15 minutes of your time. Your feedback will be used by AmeriHealth Caritas Ohio to help direct administrative and operational changes to our health plan and highlight areas of improvement. Your experience is valuable to us, and we appreciate your feedback and ongoing commitment to our members.
Thank you in advance for taking the time to participate! |
|
|---|
|
About the Provider Master File
To better serve our provider network, AmeriHealth Caritas Ohio has accepted rosters from providers as an additional level of validation against the Provider Master File (PMF) data.
Since the source of truth launch in October 2023, AmeriHealth Caritas Ohio has been monitoring its network providers and their utilization of the PMF. It has been noted that the majority of providers are now maintaining their records through the source of truth.
On August 11, AmeriHealth Caritas Ohio ceased all reconciliation efforts using rosters unless contractually obligated to do so. We encourage all providers to update their information in the PNM to ensure the most up to date information.
Best practices to ensure accurate payment and directory information
- Make sure provider records are current in the Provider Network Management (PNM) module.
- Providers should review and update their information regularly in the PNM module. AmeriHealth Caritas Ohio suggests at least monthly to avoid any payment issues.
- Provider specialties should be updated and captured as well as primary locations.
- When making changes, AmeriHealth Caritas Ohio recommends that providers allow time for updates from the PNM to populate in the Provider Master File.
- ODM can take up to 14 business days to approve and send changes to MCOs.
- If you are having difficulties getting your claims to AmeriHealth Caritas Ohio through the Fiscal Intermediary (FI), contact the Integrated Helpdesk at ODM 1-800-686-1516 or at IHD@Medicaid.ohio.gov.
- Providers can always request a reconciliation roster from their Provider Services Account Executive to make sure that data is being correctly reflected within our system and directories.
- Review panel changes, or your ability to accept new patients with your account representative to reduce patient abrasion.
|
|
Electronic Visit Verification denial codes are live!
As a reminder, denial codes are live for Home Health services, Private Duty nursing services and other home-based nurse services. For more information about electronic visit verification (EVV), you can visit our website, ODMs Electronic Visit Verification page, or call us at 1-833-644-6001.
Your claims requiring electronic visit verification must have a matching EVV visit record in Sandata. Claims that do not match will be denied.
Upcoming changes will include nurse assessment and consult services billed to managed care organizations (MCOs). As we continue to implement changes to Ohio’s EVV program, it is essential that you remain aware of the potential implications for your claim submissions.
|
Service Description
|
Service Code
|
|
Private Duty Nursing
|
T1000
|
|
Nurse Assessment and Consult
|
T1001, T1001_U9
|
Daily office hours, training webinars, and online resources are available to you. Look for emails announcing trainings from HHA/Sandata and visit Medicaid.ohio.gov/EVV for more tools to help you transition smoothly.
As this change goes into effect, remember:
- Review Guidelines: Familiarize yourself with EVV requirements and guidelines. Ensure that you and your staff are trained and equipped to handle these changes effectively.
- Verify Claim Submissions: Double-check that all claims are submitted with correct data that matches with a captured visit, including service dates, provider ID, and recipient information. Missing or incorrect data will lead to denials.
- Utilize Available Resources: Take advantage of training sessions, webinars, or resources provided by our organization and ODM to help you navigate EVV.
- Monitor Claims Status: Regularly check the status of your claim submissions to identify any issues early. Prompt action can often resolve potential problems before they escalate.
You can find all the resources mentioned above at Medicaid.ohio.gov/EVV. If you have any questions or need further clarification on EVV claims processing changes, please do not hesitate to reach out to the EVV Provider Hotline at 1-855-805-3505. You can also call or email the ODM Integrated Help Desk (IHD) at 1-800-686-1516 or IHD@medicaid.ohio.gov.
Our goal is to support you through this transition and ensure that you are fully informed about the changes that may impact your claims. We appreciate your cooperation and commitment to providing high-quality services to our members. If you have questions or concerns, please contact AmeriHealth Caritas Ohio at 1-833-644-6001.
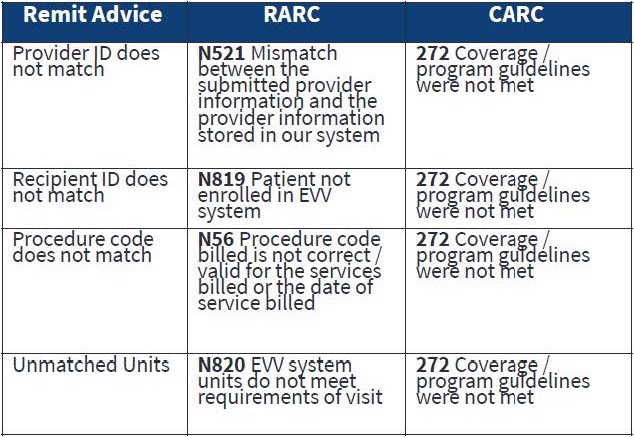
Please note the services and provider types that are subject to Electronic Visit Verification and the corresponding implementation phases. All providers must comply with ODM policy around verification, or they could experience denials.
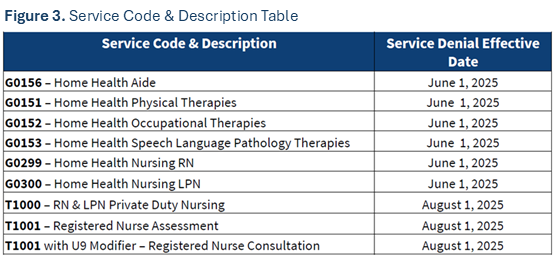
|
|
Ohio Department of Medicaid (ODM) updates
To stay up to date on ODM news, subscribe to the ODM Press.
Tips for contacting the Ohio Medicaid Integrated Helpdesk
The Integrated Helpdesk (IHD) is a great resource to use when you run into an issue. It provides 24-hour, seven days a week access to information regarding client eligibility, claim and payment status, and provider information. Read the useful tips in this newsletter.
Important reminder: Update 1099 address information in the Provider Network Management module
It is important that providers update all 1099 address information in the Provider Network Management (PNM) module regularly. Ensure all information is current, including extra address details like suite number, house/office number, etc. to reduce the chance of non-delivery by the postal service. Access the quick reference guides here.
New features implemented in the Ohio Medicaid Enterprise System
The New Features Implementation Overview outlines key changes for providers.
Medicaid agreement revalidations
To complete revalidation, visit PNM & Centralized Credentialing.
Ohio Department of Medicaid fraud warning
If your Medicaid patient is contacted for their personal information, advise them not to respond. Report it to the Ohio Attorney General at 1-800-282-0515 or via the online form.
Updated claim submission and adjudication FAQ
Claims and Prior Authorization Submission Frequently Asked Questions (FAQ).
|
|
|---|
|
Ohio Department of Medicaid email links
|
|
|---|
|
 Claims and billing Claims and billing |
|
|---|
|
Electronic claims
AmeriHealth Caritas Ohio providers have the option of submitting electronic claims via:
- Optum/Change Healthcare
- Providers with a software vendor or who use another clearinghouse to submit claims to Optum/Change Healthcare must consult their vendor/clearinghouse to confirm the process for claim submission. Please note: the 275 Claim Attachment transaction is currently available via Optum/Change Healthcare.
- Availity
- Providers or clearinghouses not currently using Availity to submit claims, must register here. Please note: The 275 Claim Attachment transaction is currently available via Availity.
Providers with Electronic Data Interchange (EDI) capabilities may submit claims, eligibility inquiries, claim status inquiries, and associated attachments, using EDI by being a trading partner (TP) authorized by ODM or by contracting with an ODM-authorized TP. For more information, visit ODM's website.
Manual/direct entry claims
Providers may submit manual/direct entry claims via:
- Optum/Change Healthcare ConnectCenter™
- This option is currently only available for providers who had an established account prior to the security incident. Access to the portal and usernames will remain the same but a password reset, and multi-factor authentication are required.
- PCH Global
Direct Data Entry (DDE) providers should submit claims via the AmeriHealth Caritas NaviNet Provider Portal. Visit our claims and billing page for more information.
How do I know when to file a new claim vs. a corrected claim?
File a New Claim when:
- The claim was never previously billed.
- Received a rejection notice at your electronic claim clearinghouse (277CA) indicating invalid or missing a required data element.
- The original claim denied for primary carrier EOB and now you have the primary carrier EOB.
- The claim denied for eligibility and now the eligibility has been updated, and the member has active coverage.
File a Corrected Claim when:
- You received a full or partial payment on a claim, but you identified that information must be corrected (some examples: billed wrong # of units, missing claim line, updates to charge amounts, adding a modifier).
- You submitted a claim for the wrong member. Submit a frequency code 8 and request a void of the original submission.
Providers using electronic data interchange (EDI) are required to submit “Professional” corrected claims* electronically.
- Corrected claims are resubmissions of an existing claim with a specific change that you have made, such as changes to CPT codes, diagnosis codes or billed amounts. It is not a request to review the processing of a claim. The successful submission of a corrected claim will cause the retraction and complete replacement of the original claim.
Your EDI clearinghouse or vendor needs to:
- Use “7” for replacement of a prior claim utilizing bill type in loop 2300, CLM05-03 (837P). Use “8” to void a prior claim.
- Include the original claim number in loop 2300, segment REF01=F8 and REF02=the original claim number; no dashes or spaces.
- Do include the plan’s claim number in order to submit your claim with the 7 or 8.
- Corrected claims for which the original claim number cannot be validated will be rejected.
- Do use this indicator for claims that were previously processed (approved or denied)
- Do Not use this indicator if the corrected claim is for a different member ID or Provider Tax ID. The original claim must be voided, and a new claim submitted for these situations.
- Do not use this indicator for claims that contained errors and were not processed (rejected upfront)
Providers using electronic data interchange (EDI) are required to submit “Institutional” corrected claims electronically Your EDI clearinghouse or vendor needs to:
- Use “7” for replacement of a prior claim utilizing bill type in loop 2300, CLM05-03 (837P). Use “8” to void a prior claim.
- Include the original claim number in Loop 2300, segment REF01=F8 and REF02=the original claim number; no dashes or spaces.
- Do include the plan’s claim number in order to submit your claim with the 7 or 8.
- Corrected claims for which the original claim number cannot be validated will be rejected.
- Do use this indicator for claims that were previously processed (approved or denied).
- Do Not use this indicator if the corrected claim is for a different member ID or Provider Tax ID. The original claim must be voided, and a new claim submitted for these situations.
- Do not use this indicator for claims that contained errors and were not processed (rejected upfront).
- Do not submit corrected claims electronically and via paper at the same time.
- For more information, please contact the EDI Hotline at 1-866-334-6446 or edi.oh@amerihealthcaritasoh.com.
- Providers using our NaviNet portal, (www.navinet.net) can view their corrected claims. You may open a claims investigation via NaviNet with the claims adjustment inquiry function.
Claims originally rejected for missing or invalid data elements must be corrected and re-submitted within 180 calendar days from the date of rejection or 365 days from date of service provided. Rejected claims are not registered as received in the claim processing system.
Before resubmitting claims, check the status of both your original and corrected claims online at www.navinet.net. You may open a claims investigation via NaviNet with the claims adjustment inquiry function.
Corrected Professional claims must be resubmitted electronically using the appropriate bill type to indicate that it is a corrected claim.
Provider NPI number validation is not performed at Change Healthcare. Change Healthcare will reject claims for provider NPI only if the provider number fields are empty. The Plan’s Provider ID is recommended as follows: 837P – Loop 2310B, REF*G2[PIN] 837I – Loop 2310A, REF*G2 [PIN].
No paper claims
The Next Generation of Ohio Medicaid program's guidelines require all claims to be submitted via the Electronic Data Exchange (EDI). Use AmeriHealth Caritas Ohio’s EDI Payer ID# 35374. You can get started on our website with claims how-tos, quick guides, links, and contact info.
Electronic funds transfer
AmeriHealth Caritas Ohio has contracted with Change Healthcare and ECHO® Health, Inc., to administer electronic funds transfer (EFT) payments. There are no fees for single payer agreements to receive a direct payment from AmeriHealth Caritas Ohio via EFT or to receive an electronic remittance advice (ERA). Click to learn how to enroll, the payment schedule, and more.
Questions about reimbursement or payment policies?
Click the appropriate link below for more detailed information.
Claims Payment Systemic Error report
The Claims Payment Systemic Errors (CPSE) report is updated and posted monthly on our website. AmeriHealth Caritas Ohio encourages you to review this log frequently and before contacting our Provider Services team. If you have additional questions, please reach out to Provider Services at 1-833-644-6001 and, as always, you can reach out to your local account executive.
Disputes and appeals
If a provider disagrees with the outcome of a claim, the first step should always be to submit a claim dispute.
Provider Disputes
Provider claim disputes are any provider inquiries or requests for reconsiderations, ranging from general questions about a claim to a provider disagreeing with a claim denial. Provider Dispute Submission Form (PDF)
A dispute can be submitted using any of the following methods:
- NaviNet (recommended method): Providers can submit a dispute with attachments to AmeriHealth Caritas Ohio via NaviNet instead of faxing or mailing. Log in, go to Forms & Dashboards, scroll down to Provider Disputes, click the Submit Provider Disputes link. The turnaround time is 15 days for disputes.
- Mail the form with your supporting documentation to:
AmeriHealth Caritas Ohio
Attn: Provider Claim Inquiry
P.O. Box 7126
London, KY 40742
- Phone: 1-833-644-6001. Select the prompts for the correct department and then select the prompt for claim issues.
- Fax: 1-833-216-2272
Provider Appeals
Providers may file an appeal on a denied pre-service within 30 days of the notice of Adverse Benefit Determination (ABD). Provider Appeal Form (PDF)
- Mail the form with your supporting documentation to:
AmeriHealth Caritas Ohio
Attn: Provider Claim Inquiry
P.O. Box 7400
London, KY 40742
- Fax: 1-833-564-1329
Questions
If you have questions about this communication, please contact your Provider Account Executive or the Provider Services department at 1-833-644-6001.
|
|
|
Single Maintenance and Reliever Therapy (SMART) is a strongly recommended practice for patients four years of age and older with moderate to severe asthma. SMART therapy uses one inhaler for both maintenance and rescue and may improve outcomes by removing the risk of mistaking one inhaler for the other.
|
|
|---|
|
 Prior authorizations Prior authorizations |
|
|---|
|
Important Update: Prior Authorization Requirements
There are no changes to home and community-based waiver processes, nor to managed care processes.
Beginning August 1, the Ohio Department of Medicaid began denying claims submitted without an approved prior authorization under the Fee-For-Service (FFS) policy. This change is critical to ensure compliance with Ohio Medicaid’s updated requirements.
You can read the entire press release, learn more about the PNM module and prior authorization, and register for training by clicking here.
Out of network providers
Contact Utilization Management for a prior authorization before providing care to our members: 1-833-735-7700. If you are interested in joining our network, contact our contracting department: providerrecruitmentoh@amerihealthcaritasoh.com. This email address can also be used by vision providers looking for in-network vendors who can provide eyeglass frames and lenses.
Submit prior authorization requests (PA) electronically through NaviNet
AmeriHealth Caritas Ohio offers our providers access to our Medical Authorizations portal for electronic authorization inquiries and submission. The portal is accessed through NaviNet and located on the Workflows menu.
In addition to submitting and inquiring on existing authorizations, you will also be able to:
- Verify if no authorization is required
- Receive auto approvals, in some circumstances
- Submit amended authorization
- Attach supplemental documentation
- Sign up for in-app status change notifications directly from the health plan
- Access a multi-payer authorization log
- Submit inpatient concurrent reviews online if you have health information exchange (HIE) capabilities (fax is no longer required)
- Review inpatient admission notifications and provide supporting clinical documentation
Submit all medical pharmacy prior authorizations (PA) to PerformRx
Prior authorization requests for prescriber administered medications should be submitted to PerformRx via fax. See our website for more information and the form.
|
|
Working with you to build healthy communities
Are you interested in working with us to reach and engage your community members? Would you like to have our mobile unit at your community event? For more information about reserving time in our Mobile Wellness and Opportunity Center, please complete our online form. |
|
|
|
|
 For behavioral health providers For behavioral health providers |
|
|---|
|
AmeriHealth Caritas Ohio is offering FREE training with pre-approved CEUs
This course will provide the Ethics and Rules from Ohio Law regarding the direction of Suicide Prevention, Intervention, and Postvention Care. It will also introduce and discuss the Ethics of Trauma Sensitive Care for Suicide and Crisis Focused Care. Cultural considerations for marginalized populations will be addressed. We will provide opportunities for case conceptualization and treatment planning.
- Ethics of Providing Trauma Sensitive Suicide Prevention Focused Care
- September 25, 8:30 a.m. to 11:45 a.m.
- 3.0 pre-approved CEUs for Ohio counselors, social workers, and marriage and family therapists.
|
|
|---|
|
CEU opportunities
Sign up to receive email about AmeriHealth Caritas Ohio’s free Continuing Education Unit (CEU) opportunities.
Submitting prior authorization (PA) requests for behavioral health services
See the tip sheet for guidance on submitting PAs for behavioral health service requests. |
|
|---|
|
Resource for behavioral health consultations launching for primary care providers
In July, the Ohio Pediatric Psychiatry Access Line (OPPAL) launched, offering pediatric primary care providers in Ohio access to a telephone helpline for same day, convenient peer to peer consultation with child psychiatrists. Learn about OPPAL by clicking here.
|
|
|---|
|
 Resources and reminders Resources and reminders |
|
|---|
|
New vendor to provide in-home health evaluations (IHE)
AmeriHealth Caritas Ohio works with you to collect complete and accurate member health histories to help facilitate care management, as appropriate. As part of these efforts, we are partnering with Signify Health to conduct In-Home Health Evaluation (IHE) visits to assist us in documenting our member's/your patient’s healthcare conditions, diseases and other social demographic related factors. Read all of the details here.
Multi-Factor authentication for Care Coordination Portal access
To increase protection for the Managed Care Organization Care Coordination Portal’s and member information data, signing in will soon require Multi-Factor Authentication (MFA). MFA is a two-factor authentication process that takes user verification a step beyond the State of Ohio (OHID) and password. This is done by using a second source of validation (i.e., text message, email, passkey, phone call) to verify user identify before granting access.
Did you know?
- You can submit prior authorization requests on our secure provider portal NaviNet, and in some instances receive auto-approval. Turnaround times are faster when using NaviNet.
- In the event you are unable to request a prior authorization, you can request a retro authorization if there is no claim on file. If no claim is on file, UM will review retro requests. Please contact your dedicated Account Executive with questions.
Chronic condition management — blood pressure collection
AmeriHealth Caritas Ohio periodically performs member outreach to complete screening assessments and coordinate care with our members to improve the health outcomes of our members.
When a member measures their blood pressure using a digital in-home monitor during outreach with our care management staff, we will send you a letter summarizing the results. Click to view the summary chart that you will receive.
Reducing disparities in the management of hypertension in African American members
This toolkit covers topics such as barriers to care within the African American population and supportive best practices, tools, and strategies when working to reduce high blood pressure for your African American patient population.
Sign up for this newsletter
Our monthly newsletter, Provider Partnerships, keeps you informed about plan news, updates, and resources. Click here to sign up.
Member rights and responsibilities
AmeriHealth Caritas Ohio members have rights and responsibilities. We believe all members have the right to receive information on the services AmeriHealth Caritas must provide, the right to be treated with respect, dignity, and privacy.
- Members have the right to receive medically necessary treatment options for their conditions no matter the cost or benefit coverage.
- Members are to take part in decisions about their healthcare.
- Members are to treat healthcare staff with respect, be aware of the benefits and services available to them.
- Ask for more explanations if they do not understand their doctors' instructions.
- To provide their physicians with accurate and complete medical information.
Redeterminations
We understand that many members may be unaware that their redetermination period is approaching, and your engagement can play a crucial role in ensuring they take the necessary steps to avoid a lapse in coverage. We encourage our providers to remind their patients that they may need to complete the redetermination process to help ensure they can retain their Medicaid benefits.
Please let us know how we can support you in sharing this important information. We appreciate your partnership and commitment to member health and continuity of care.
Provider resources
We highly recommend providers take a few minutes to familiarize themselves with the tools available on our website. Our user-friendly tools and resources are designed to support Ohio’s Medicaid providers and your staff in giving members excellent and efficient healthcare.
- prior authorization lookup tool
- video tutorials for claims submission
- step-by-step instructions for claims submission and our secure provider portal NaviNet
- Provider Manual
- Provider Claims and Billing Manual
- contact information for our call center and AmeriHealth Caritas Ohio provider services
- monthly CPSE reports and trending claims issue information
Updated HEDIS guidelines for the Care Gap Closure program
View the HEDIS 2024 Documentation and Coding Guidelines for care delivered in 2024.
Provider Network Management (PNM) portal
Until it is fully active, please continue to send roster updates to both PNM and the MCO’s. Behavioral Health providers ARE able to only update through the PNM portal without submitting rosters to the MCO’s.
Credentialing reminder
Providers no longer need to complete credentialing with each managed care organization. Credentialing is now completed through the state's PNM portal. More information can be found here.
|
|
 Training opportunities Training opportunities |
|
|---|
|
ODM required annual EPSDT education
AmeriHealth Caritas Ohio provides this Healthchek education to all contracted providers on an annual basis.
The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit provides comprehensive and preventative healthcare services for children under age 21 who are enrolled in Ohio Medicaid. Healthchek covers 10 checkups in the first two years of life and annual checkups after age three.
EPSDT benefits includes a range of medically necessary screening, diagnostic, and treatment services to prevent, diagnose, treat, evaluate, correct, or ameliorate adverse health conditions including illness, injury, emotional or behavioral dysfunction, intellectual deficits, cognitive impairments, or developmental disabilities.
EPSDT is key to ensuring that children and adolescents receive appropriate preventative, dental, mental health, developmental, AND specialty services.
Screenings must include:
- Comprehensive health and developmental history
- Comprehensive unclothed physical exam
- Laboratory Tests – including lead toxicity screening as guided by the child’s age
- Appropriate and needed immunizations
- Health Education – anticipatory guidance including child development, healthy lifestyles, and accident and disease prevention
- Vision Services – at minimum, diagnosis, and treatment for defects in vision, including eyeglasses
- Dental Services – at minimum, relief of pain and infections, restoration of teeth, and maintenance of dental health
- Hearing Services – at minimum, diagnosis and treatment for defects in hearing, including hearing aids
- Nutrition assessment and education
- Other necessary health care services – diagnostic and treatment services must be provided when a screening examination indicates the need for further evaluation
The Well Child Visit Schedule recommended by American Academy of Pediatrics (AAP) is listed below. To view the comprehensive Periodicity Schedule for Preventative Health Care, click here.
|
|
|---|
|
Virtual office hours
Got Questions? Let us help you. Join the ACOH Provider Services team for a virtual office hour. Our team will be here to help answer your questions or help you navigate our provider resources. No registration is necessary. Just click here to join on any of these dates:
|
|
|
|
Tuesday, August 26
|
Noon to 1 p.m.
|
NaviNet
|
|
Friday, September 26
Friday, October 24
|
Noon to 1 p.m.
Noon to 1 p.m.
|
Population Health & Care Coordinators
Medicaid Renewal and Redetermination
|
|
|
|---|
|
Provider orientation
AmeriHealth Caritas Ohio invites you and your staff to join us for a virtual New Provider Orientation session. Your personal AmeriHealth Caritas Ohio Account Executive looks forward to meeting you!
Tuesday, September 16
10 a.m. - 11 a.m.
Click to register
Click here to see the entire calendar.
|
|
|---|
|
All-MCO doula technical assistance trainings
Ohio's seven Medicaid Managed Care Organizations (MCOs), in partnership with the Ohio Department of Medicaid, are hosting a virtual technical assistance training series for doulas.
Training session 1: August 28, 10 a.m. to 11:30 a.m.
The first session will provide information on the following topics:
- Contracting process with MCOs
- Verifying Medicaid eligibility for members
- Submitting accurate electronic claims through the MCO provider portals
- Correct billing procedures including diagnosis codes
- Guidance on completing the Report of Pregnancy (ROP) in NurtureOhio
- Ways to obtain help/support from the MCOs
This practical session emphasizes proper documentation and compliance with Medicaid managed care rules for billing doula services. Strengthen your practice and gain confidence in navigating Ohio’s Medicaid Managed Care system. We look forward to working with you to improve maternal and infant support throughout Ohio.
Training session 2: November 3, 2 p.m. to 3:30 p.m.
Details regarding the second session will be sent closer to the training.
|
|
|---|
|
Comprehensive Primary Care (CPC) quarterly webinar series
The 2025 CPC quarterly webinar series will focus on keeping practices informed about the latest CPC updates, learning opportunities, discussions and more. Topics will be sent out ahead of time. Click here to register.
These take place from 9:30 a.m. to 11 a.m. on the following dates:
- Tuesday, September 16
- Tuesday, November 18
For those who are unable to attend the webinars, the presentations along with a brief description of the covered webinar topics will be posted to the CPC Webinars and Trainings webpage. It is important that all CPC practices attend the webinar sessions, or at a minimum, review the posted presentations. Doing so keeps our practices up to date on all things CPC.
|
|
|---|
|
Cultural competency training opportunities
AmeriHealth Caritas Ohio is committed to promoting education and awareness of culturally and linguistically appropriate services (CLAS) and to combatting the effects of low health literacy on the health status of our members. |
|
|---|
|
Tell us a little bit about where you’re from and where you went to school.
I was born and raised on the West Side of Columbus, also called the Hilltop. I attended Highland Avenue Elementary, Hilltonia Junior High School and West High School. Go Cowboys!
Everyone at AmeriHealth Caritas Ohio has a story about why they joined the team. What’s yours?
I joined this team based on my discussions with Mr. Russ (Mr. Mark’s boss) and Mr. Mark Grippi. Both spoke of the AmeriHealth Caritas Family of Companies mission and vision. More importantly, there was a passion from them both to be member focused. As the incoming Director of Member Engagement, I shared their passion to be member focused.
The two most important days of your life: the day you were born and the day you find out why! UHCAN Ohio provided my "why" at the 2024 Lend Your Voice – Health Care for All Annual Tribute as one of six honorees. It was the culmination of my "why" and my current work. |
|
|
What drew you to this profession?
Universal Health Care Action Network (UHCAN) of Ohio hired me as their Director of Community Outreach. As a result, the role linked me to contracting with Ohio Department of Medicaid and Centers for Medicare & Medicaid Services to roll out the MyCare Ohio program. I grew to love the MyCare role, especially engaging members to ensure they were receiving the services and support they so richly deserved.
What do you like to do in your free time?
Read and go dancing with my wife.
If you could have dinner with anyone in the world, dead or alive, who would it be? Why?
My dad. He has gone to be with the Lord. I would want to see and hear if he is still proud of me and if I met his expectations for the life he envisioned for me.
What are 2 apps on your phone you CANNOT live without?
Only one - Pandora.
Any interesting facts about yourself that you’d like to share?
I was the very first of the Arnold and Henley family lineage to graduate from college and obtain a master's degree.
John E. Arnold
Director, Member Engagement & Community Relations
1-614-515-8307
|
|
|---|
|
Celebrate National Wellness Month during the entire month of August. It's time to prioritize your self care, reduce stress, and create healthier habits to feel like your best self. It's easy to put our health and wellness on the back burner due to work deadlines, traffic, family obligations and other stressors. Research has shown self care can help increase happiness by up to 71% when we manage our stress and maintain a healthy lifestyle. In fact, self care helps manage stress and promotes happiness. Whether you challenge yourself to a new yoga pose or try a different spa treatment, make a small change and impact your health in positive ways.
5 Wellness Tips
Taking small steps to improve your personal wellness will lead to healthy habits in your lifestyle. In fact, wellness changes don't have to be life changing, even though the
|
|
|
|
|---|
|
long-term results will be. You can improve your overall health by:
- Increasing your water intake
- Adding more fruits and veggies to your meals
- Monitoring your sleep and making adjustments for better sleep habits
- Joining a yoga, walking, or aerobics class
- Learning to meditate
|
|
|---|
|
Need help?
AmeriHealth Caritas Ohio Provider Services is ready to help.
|
|
|---|
|
|
|
|
|  |
|
|
|
|
